THERMAL ABLATION
The gentle treatment of benign thyroid nodules with impressive advantages: effective, function-preserving and low-complication minimally invasive method without a surgical scar.

Representation of thyroid ablation with a special thermal probe, at the tip of which heat is generated, which cauterizes the nodular altered thyroid tissue. In the following weeks, it will be metabolized by the body's own immune system.
WHAT IS A THERMAL ABLATION?
Thermal ablation of thyroid nodules by radiofrequency was developed more than 15 years ago and has been used in several European countries for multiple years. Now, this minimally invasive method is also available in Switzerland. The term thermal ablation is used to describe processes in which tissue is cauterized by heat. Irreversible cell damage occurs beginning at temperatures above 60 degrees Celsius. In thermal ablation - similar to a biopsy - a special thermal probe is inserted into the thyroid nodule under ultrasound control and destroys the nodule by selective heating of the probe tip. There are no nerve fibers in thyroid nodules, so the procedure, which is performed under local anesthesia, is very painless and does not require general anesthesia. The cauterized tissue is broken down by the body and the nodule shrinks. This shrinking process depends on the composition of the nodule and ranges between 60 - 90% within one year.
WHAT ARE THE ADVANTAGES OF THERMAL ABLATION?
· minimally invasive procedure without scarring with an intervention duration of 15 - 60 min
· no general anesthesia necessary, therefore no anesthesia-related risks
· function-preserving procedure: the intake of thyroid medication to support thyroid function as it is often the case after a surgery is not to be expected after a thyroid ablation since the healthy thyroid tissue is spared
· high effectiveness: the size reduction of a treated nodule is - depending on its composition - between 60-90% (approx. 80% on average) after one year
· very low complication rate: particularly the relevant operative risks such as permanent damage to the vocal cord nerve or parathyroid are not to be expected
WHAT IS THE EXACT PROCESS OF A THERMAL ABLATION?
The procedure does not require general anesthesia, i.e. patients come to the surgery room after appropriate preparation and take a seat on the examination table. Subsequently, grounding pads are glued to the front of both thighs and a small device for measuring the oxygen saturation in the blood is attached to the fingertip. Then the patient is covered with sterile cloths, the neck is disinfected and the head is placed in a slightly overstretched position with a small cushion. The patient can breathe, swallow and speak normally during the whole process of sclerotherapy. The doctor will then use a very thin needle to place a local anesthetic under the skin and ultrasonically target the thyroid capsule so that the subsequent procedure is not painful in the vast majority of cases. This is because the thyroid gland itself is not sensitive to pain, contrary to the surrounding capsule which is anesthetized.
Then the actual sclerotherapy probe is inserted into the nodules. A generator generates an alternating electromagnetic field directly at the end of the needle tip. This way, the nodule tissue is heated a few millimeters around the probe tip and treated point by point. Each sclerotherapy level is treated until the entire nodule tissue has been covered. The generator as well as the water pump work with a certain background noise and "cracking" noises (like when making popcorn) occur often during sclerotherapy but are completely harmless. Depending on the size and number of nodules to be treated, the procedure takes about 15-60 minutes. Subsequently, the patient receives a small patch on the puncture site and the treated neck region is cooled with ice packs.

Illustration of a cross-section through the neck and thyroid region. The needle creates small heat fields around its tip, which cause the nodule to cauterize point by point.

Puncture site 1 month after thermal ablation, via which a thyroid gland nodule can usually be completely treated. Relevant optically visible scars therefore do not occur.
WHAT SHOULD BE OBSERVED AFTER A THERMAL ABLATION?
The procedure is so gentle that even immediately after the procedure and in the first few days after it, the vast majority of patients have little or no discomfort. As a rule, one puncture of the skin is also sufficient to treat the entire thyroid gland. In the 3 days following the surgery, avoid lifting heavy objects (over 5 kg), strenuous physical and sporting activities in general as well as maneuvers associated with holding your breath (pressing) (e.g. playing wind instruments, blowing something up, etc.). Working patients are able to work again after these 3 days.
WHAT HAPPENS TO THE TREATED NODULE AFTER THERMAL ABLATION?
The sclerotic cells of a treated thyroid nodule are metabolized by the body's own immune system in the weeks following the procedure. After 2-3 weeks, patients usually notice that the nodule has already become smaller. Cystic nodules regress faster than solid nodules. After one year, the regression of the nodule is usually between 60-90%, depending on the composition of the nodule. Since the treatment converts the nodule tissue into scar tissue and there is no active thyroid tissue left, a well-treated nodule does not regrow.



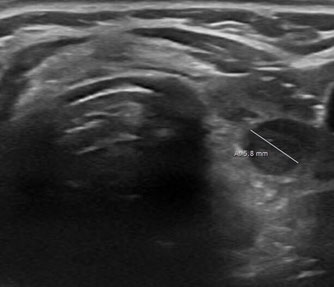
Photo and sonography of a thyroid nodule before and 6 months after thermal ablation. The nodule shows a volume reduction of approx. 90%.
WHICH PATIENTS CAN BE TREATED BY THERMAL ABLATION?
The feasibility of thermal ablation can of course only be clarified after a personal consultation with the attending physician. The method is not suitable for thyroid cancer. In principle, the following thyroid diseases are presumably considered to be treatable:
• Symptomatic benign nodule formations
• Symptomatic thyroid cysts
• Rapidly growing benign nodules or cysts
• Visually disturbing nodules or cyst formations
• "Hot" nodule formations (autonomous adenoma) when radioiodine therapy is not desired
• Patients who do not want surgery
• Patients who are only partially suitable for surgery or not fit for anesthesia
CONTACT DETAILS OF THE AUTHOR

PROF. DR. MED. OLIVER DUDECK
Interventional Radiology, FMH Radiology
Special focus Neuroradiology

Klinik Hirslanden
Witellikerstrasse 40, 8032 Zurich
Email: oliver.dudeck@hirslanden.ch
Web: www.swissintervention.ch
Phone: +41 44 387 2935
